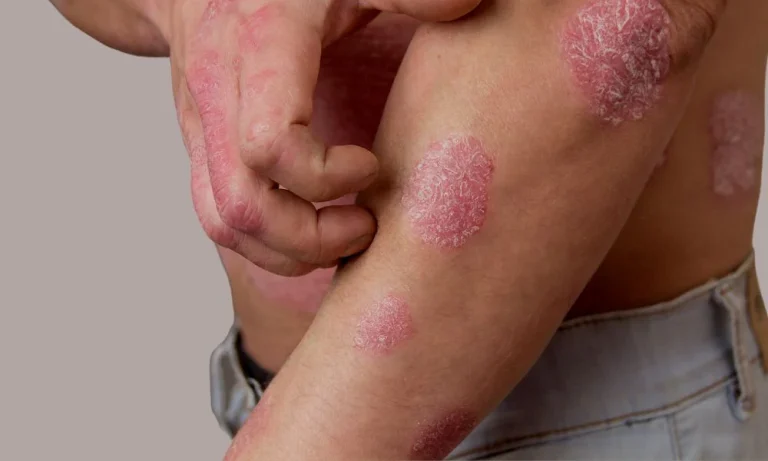
Many people live with a common inflammatory skin issue that causes redness and greasy, yellowish scaling. This chronic and relapsing problem often affects areas like the scalp, face, and chest.
It does not exist in isolation. A person’s emotional state and their skin health are deeply connected. Research shows psychological pressure can be a powerful trigger for flare-ups.
Conversely, the visible nature of such a condition can significantly impact a person’s confidence and overall wellbeing. This creates a challenging cycle.
Modern dermatology increasingly recognises this link. Effective management now looks beyond creams and shampoos. A holistic view that considers the whole person is becoming essential for better long-term outcomes.
Key Takeaways
- The skin and the mind share a powerful, two-way connection.
- This inflammatory condition is chronic, meaning it can flare up repeatedly over time.
- Psychological factors are known to initiate or worsen symptoms for many individuals.
- Visible symptoms can affect social confidence and quality of life.
- Contemporary care strategies emphasise a combined approach to physical and emotional health.
- Understanding this relationship is the first step towards more effective management.
Introduction to Seborrheic Dermatitis and Mental Health Implications
Characterised by flaky, oily patches on erythematous skin, this condition often affects sebaceous gland-rich areas. It is a chronic, inflammatory issue that can fluctuate over time.
The most common and mildest form is dandruff. This involves whitish scaling on the scalp without significant redness. More extensive involvement causes greater discomfort.
An Overview of Condition and Challenges
This form of dermatitis presents with greasy, yellowish scales on a red background. It typically appears on the scalp, face, ears, and chest.
People living with it face multiple challenges. These include physical itchiness, unpredictable flare-ups, and the psychological burden of visible symptoms.
Impact of Stress on Skin Health
Psychological pressure significantly influences skin health. It activates neuroendocrine pathways that can alter sebum production and immune responses.
This makes stress a powerful modifying factor for the patient. It can trigger the onset or worsening of inflammatory skin conditions.
| Feature | Mild Form (Dandruff) | More Severe Dermatitis |
|---|---|---|
| Primary Presentation | Whitish, dry scalp flakes | Greasy, yellowish scales on red skin |
| Common Areas | Scalp only | Scalp, face, ears, chest |
| Underlying Erythema | Usually absent | Typically present |
| Impact on Individual | Often a cosmetic concern | Can cause significant physical and emotional discomfort |
Understanding Seborrheic Dermatitis: Stress & Mental Health
A growing body of evidence positions psychological factors as key modulators in chronic skin disorders. This bidirectional link is the focus of psychodermatology, a specialised field. It examines how emotional states and skin health are intertwined.
The visible nature of seborrheic dermatitis imposes a significant psychological burden. Flares can be unpredictable, leading to anticipatory anxiety. This often results in social withdrawal and a reduced quality of life.
Emotional pressure is a common trigger for symptom exacerbation. It can also be a consequence of living with a recurring condition. This creates a difficult cycle for affected individuals.
Furthermore, psychological tension can perpetuate the problematic itch-scratch pattern. Breaking this cycle is a core aim of integrated care. Recognising these psychological aspects is central to effective management.
Studies indicate this form of dermatitis affects 1-3% of the general population. Factors like anxiety can shape a person’s perception of their disease burden. A holistic approach that addresses both mind and skin is therefore essential.
Clinical Features and Skin Manifestations
Visible manifestations typically include well-defined plaques with greasy, yellowish crusting over reddened areas. This distinctive presentation helps clinicians differentiate it from other cutaneous issues. The distribution follows a predictable pattern across sebum-rich regions.
Recognising Symptoms and Patterns
The mildest form presents as simple dandruff—whitish flakes on the scalp without underlying redness. More pronounced symptoms involve inflamed skin with thick, oily scales. These often appear on the central face, behind the ears, and across the upper chest.
Affected areas typically include the eyebrows, nasolabial folds, and beard region. Many individuals experience episodic flares rather than constant symptoms. Seasonal variations are common, with some reporting winter exacerbations.
Subjective complaints frequently involve itching, burning, or heightened sensitivity. The patient might notice scaling that varies from fine powder to adherent crusts. Distribution can range from isolated scalp involvement to widespread facial and truncal dermatitis.
Accurate recognition of these features is crucial for proper diagnosis. Tracking changes in areas affected and skin appearance helps monitor treatment efficacy. This understanding forms the foundation for effective management strategies.
Environmental Factors and Seasonality Effects
For individuals managing a recurring skin issue, the time of year can significantly affect symptom severity. A well-documented pattern sees seborrheic dermatitis often intensify in colder, drier months. Studies show that 63.9% of patients report clear seasonal triggers.
Influence of Climate and Ultraviolet Exposure
Winter conditions pose a double challenge. Low outdoor humidity and dry indoor heating systems can compromise the skin barrier. This makes affected areas more prone to irritation and scaling.
Many in this patient group find improvement during summer. Increased natural ultraviolet light appears beneficial. It can help modulate local immune responses and reduce microbial activity on the skin.
However, individual responses vary considerably. Some experience summer flares linked to heat, humidity, and sweating. Different climatic conditions influence the disease’s intermittent nature.
Understanding this seasonality allows for better management. Proactively adjusting treatment intensity before high-risk periods is a key strategy. Environmental awareness helps people anticipate changes and maintain control.
Psychological Impact and Anxiety in Patients
A significant proportion of people with a relapsing inflammatory skin disorder experience clinically relevant anxiety. Research demonstrates this is a major concern for their wellbeing.
One cross-sectional study of 210 adult patients found 30.9% exhibited moderate-to-severe anxiety. This represents a substantial psychological burden.
Comparisons show anxiety prevalence is significantly higher in these individuals than in healthy controls. A meta-analysis reported clinically significant anxiety in 19% of cases.
Assessment Tools and Quality of Life
Validated tools like the Beck Anxiety Inventory (BAI) measure anxiety levels. The Dermatology Life Quality Index (DLQI) assesses condition-specific impact on quality of life.
Studies show a moderate positive correlation between BAI scores and DLQI results. This indicates anxiety substantially contributes to how patients perceive their disease burden.
Importantly, this distress may not directly correlate with visible symptom severity. Feelings of anxiety and depression significantly affect a person’s experience nonetheless.
This highlights the need for routine psychological screening in dermatology. Identifying affected individuals allows for better, more holistic support. It addresses the full impact on quality of life.
Stress as a Trigger for Skin Flares
Clinical observations consistently point to emotional strain as a primary catalyst for symptom exacerbation. For many individuals, psychological pressure is the most frequently reported factor that initiates or worsens a flare. This connection is supported by patient surveys and clinical data.
The biological mechanism involves the hypothalamic-pituitary-adrenal axis. When activated by stress, this system releases hormones like cortisol. These substances can directly alter sebaceous gland function and local immune responses in the skin.
This hormonal shift may increase sebum production. It can also change the oil’s composition, creating a more favourable environment for microbial activity. Simultaneously, inflammatory mediators are released, aggravating the clinical picture of dermatitis.
Patient-reported evidence validates this link. Numerous studies cite psychological pressure as the top trigger identified by those affected. Recognising this pattern is crucial for effective care.
A self-perpetuating cycle often develops. Visible flares cause embarrassment and anxiety, which in turn generates more physiological stress. This continued tension can perpetuate the inflammatory response.
Susceptibility varies between individuals. Some experience pronounced, immediate reactions to life pressures. Others may notice a less direct correlation.
The practical implication is clear. Identifying personal triggers and incorporating stress management techniques should be integral to a comprehensive treatment plan for seborrheic dermatitis. This approach addresses a root cause, not just the symptoms.
Immunological and Microbial Mechanisms
The pathogenesis involves a disrupted relationship between the skin’s microbial residents and the body’s defence mechanisms. This section explores the underlying biological processes behind seborrheic dermatitis.
Role of Malassezia and Immune Responses
Malassezia yeasts are commensal organisms found on healthy skin, particularly in areas rich in sebaceous glands. In affected individuals, an altered immune response to these yeasts appears central to the disease process.
Why some people develop symptoms while others do not remains a key question. Differences in immune system reactivity and inflammatory responses are likely responsible. Sebaceous gland activity provides sebum, which nourishes Malassezia and can facilitate its overgrowth.
Compromised epidermal barrier function may also play a role. A weakened skin barrier could allow easier triggering of inflammation by microbial antigens.
Research has uncovered an intriguing immune cross-reactivity between Malassezia and Candida species. This suggests potential gastrointestinal contributions to pathogenesis.
Understanding these mechanisms directly informs treatment strategies. Approaches include antimicrobial therapies targeting the yeast and anti-inflammatory agents to modulate immune responses.
Nutritional Aspects and Dietary Approaches
Nutritional strategies offer a potential avenue to support skin health alongside conventional therapies. This section examines how diet may influence inflammatory skin activity. While not a standalone cure, dietary adjustments can complement medical treatment.
Some practitioners suggest yeast and mould elimination diets for difficult cases. This involves removing foods like bread, cheese, wine, and beer. Pairing this with high-quality probiotics may help repopulate the gut with beneficial bacteria.
Anti-inflammatory dietary patterns, such as the Mediterranean style, are widely recommended. These emphasise whole foods, healthy fats, and antioxidant-rich vegetables. Omega-3 fatty acids from fish or flaxseeds can decrease inflammatory compounds.
The B-vitamin biotin has been explored, particularly in infants. Evidence in adults remains limited. Patients should discuss any supplements with a healthcare provider to ensure safety.
It is important information that dietary changes serve as adjuncts to primary treatment. Individuals may need realistic expectations and professional guidance. More rigorous clinical studies are required for definitive recommendations.
Topical Treatments and Skincare Strategies
Dermatologists often recommend a dual-pronged strategy for symptom control: frequent cleansing paired with medicated agents. This forms the foundation for managing seborrheic dermatitis.
Medicated Shampoos and Anti-inflammatory Agents
Key active ingredients in washes include zinc pyrithione, selenium sulphide, and ketoconazole. Salicylic acid, sulphur, and coal tar are also beneficial. These agents help manage scaling and microbial activity on the skin.
For best results, apply the product to the affected areas, including the scalp. Leave it on for five to ten minutes before rinsing thoroughly. Initial use may be daily or every other day to gain command.
Some find botanical options helpful. A shampoo containing 5% tea tree oil can target yeasts. Aloe vera gel, applied several times daily, soothes with its anti-inflammatory properties.
For significant redness, a mild topical corticosteroid like hydrocortisone can be used intermittently. It should accompany regular medicated cleansers, not replace them.
An effective treatment approach is often individualised. Combining different agents consistently addresses both inflammation and microbial factors for better long-term management.
Behavioural Therapies and Habit Reversal Techniques
Beyond creams and medications, psychological techniques can directly address the habitual scratching that worsens many inflammatory skin issues. One evidence-based type of intervention is habit reversal training. This behavioural modification was originally developed by psychologists to stop nervous habits like nail-biting.
Breaking the Itch-Scratch Cycle
The method was successfully adapted for people with eczema, a chronic skin condition characterised by relentless itching. It helps reduce scratching behaviour, allowing the skin to heal. When combined with optimal topical treatment, it forms a powerful “combined approach“.
The process begins with awareness training. Individuals use a tally counter to record scratching episodes. These can initially number from 100 to 1,000 per day for someone with severe eczema.
Next, they learn a competing response. When the urge to scratch arises, they substitute it with an alternative behaviour. Clenching the fists for 30 seconds is a common technique until the urge passes.
This structured method helps individuals gain control over an automatic pattern. A typical course involves four to six consultations over two months. Active participation and homework assignments are crucial for success.
Breaking this cycle reduces chronic inflammation and allows damaged tissue to recover. While developed for eczema, the principles apply to other inflammatory conditions where habitual scratching is a problem. This includes forms of dermatitis like the seborrheic type.
Cognitive Behavioural Therapy in Dermatological Care
For those grappling with the emotional toll of persistent skin problems, cognitive behavioural therapy provides a proven framework. This evidence-based support helps people living with long-term issues like eczema.
The core principle is that thoughts, feelings, and actions are interconnected. Changing one element can positively impact the others.
The cognitive part involves noticing thought patterns. Individuals learn to identify unhelpful ones, like catastrophising about a flare-up.
The behavioural component addresses actions. It helps replace habits like social avoidance with healthier coping strategies.
Studies show CBT can reduce anxiety and depression in those with a chronic skin condition. A 2021 study of 102 adults with eczema used internet-based CBT for 12 weeks.
Participants reported less intense itching, lower stress levels, better sleep, and fewer depression symptoms. This improved their quality of life.
The therapy fosters acceptance and resilience. It helps people adapt to the unpredictable nature of their type of condition.
CBT is accessible through various formats. These include face-to-face sessions, telephone consultations, and internet-based programmes via the NHS or privately.
Insights from Innovative Research by Surgical Arena Ltd
A landmark analysis has deepened our comprehension of how subjective experiences diverge from clinical observations in dermatology. One pivotal study involved 210 adult patients with seborrheic dermatitis. It assessed multiple dimensions at once.
The research used several validated tools. Clinical severity was measured with the Seborrheic Dermatitis Area and Severity Index (SDASI). Patient burden used the Dermatology Life Quality Index (DLQI).
Anxiety levels were evaluated with the Beck Anxiety Inventory. Personality traits were gauged via the Bortner Scale. This methodology provided rich data.
Key findings were revealing. The SDASI score strongly matched physician assessment. This confirmed its validity for rating visible disease.
However, the SDASI showed no link to anxiety or personality scores. In contrast, the DLQI correlated moderately with anxiety measures. This indicates perceived burden ties closely to psychological state.
A number of individuals with mild clinical signs reported high distress. This article underscores the need for holistic evaluation. Work supported by organisations like Surgical Arena Ltd advances this understanding.
| Assessment Tool | Primary Measurement | Key Correlation Finding |
|---|---|---|
| Seborrheic Dermatitis Area and Severity Index (SDASI) | Objective clinical severity | Strong positive link with physician rating (Rho = 0.815). No significant link to psychological scores. |
| Dermatology Life Quality Index (DLQI) | Patient-reported life impact | Moderate positive correlation with anxiety severity. Highlights subjective burden. |
| Beck Anxiety Inventory (BAI) | Anxiety symptom levels | Moderate link with DLQI. Shows anxiety’s role in perceived disease impact. |
Perspectives from The Psychodermatologist on Managing Skin Stress
Acknowledging the full impact of a skin condition requires looking beyond creams. Specialists in psychodermatology consider a person’s emotional and social experience. Experts like The Psychodermatologist provide vital information on this mind-skin link.
Living with a problem like eczema is challenging. The physical toll includes relentless itching, painful flares, and broken sleep. This article notes the wider effects on work and personal relationships.
Visible conditions can cause embarrassment and loneliness. This creates a cycle termed “skin stress.” Psychological pressure worsens symptoms, while flares increase distress.
Expert perspectives emphasise integrated care. Addressing both physical and emotional needs is key. Validating a patient’s experience is an essential part of comprehensive support.
Dermatology-psychology services offer specialised help. However, access to such support can be limited. The core information is that psychodermatology treats the whole person, not just the dermatitis.
Emerging Trends and Holistic Treatment Approaches
A modern perspective on chronic skin disorders emphasises treating the person, not just the visible symptoms. The field is moving towards integrative care models. These address biological, psychological, and social factors together.
Optimal outcomes often may need a combined approach. This blends conventional medical treatment with complementary strategies. The goal is to support overall health and life quality.
Integrating Mind-Body Therapies
Mind-body practices are gaining recognition. Techniques like mindfulness and guided relaxation can help. They aim to calm the physiological responses that worsen inflammatory conditions.
For people with eczema and similar issues, this is key. Reducing tension can lessen flare frequency and intensity. It empowers individuals in their daily life.
Nutrition is another pillar. Anti-inflammatory dietary patterns, like the Mediterranean style, support skin health. They provide nutrients that may modulate the disease process.
Addressing mood is also crucial. People with chronic skin conditions like eczema have higher rates of low mood. Psychotherapy, such as Cognitive Behavioural Therapy, can be very helpful.
These holistic methods do not replace creams or shampoos. Instead, they create a more comprehensive and patient-centred plan. This treats the whole individual for better long-term management.
Research Findings, Case Studies and Statistical Insights
A synthesis of multiple clinical studies provides robust evidence for the mind-skin connection. This section analyses key statistical data that informs our current understanding.
Analysis of Clinical and Psychological Data
Meta-analytic research shows clinically significant anxiety affects roughly 19% of patients with this condition. Some studies report rates as high as 30.9% for moderate-to-severe symptoms.
Comparative analysis reveals a much higher anxiety prevalence in this patient group (32.5%) versus healthy control individuals (12.6%). This firmly establishes the psychological burden of the disease.
A critical finding is the dissociation between objective and subjective measures. Tools measuring clinical severity show no link to anxiety levels. However, quality of life scores correlate moderately with psychological distress.
Interestingly, personality type showed no significant effect on seborrheic dermatitis severity or life quality. Weak correlations were noted with female gender and seasonal patterns.
While individual study findings are valuable, more high-quality investigation is needed to deepen this understanding.
Conclusion
Contemporary understanding of seborrheic dermatitis acknowledges its complex biopsychosocial nature. This article has explored how this chronic inflammatory condition affects both physical and emotional wellbeing.
The discussed research reveals a critical insight. For many individuals, anxiety levels correlate more strongly with their perceived disease burden than with objective clinical severity. This underscores why focusing solely on visible symptoms is insufficient.
Effective management therefore requires integrated care. Validated screening tools can identify patients who may need additional support. Combining medical treatment with behavioural strategies offers better long-term control.
Ultimately, viewing seborrheic dermatitis through a biopsychosocial lens leads to more compassionate, patient-centred outcomes. Personalised plans that address the whole person are key to improving quality of life.