By Draper Spinal Care | Draper, Utah
When patients visit Draper Spinal Care for the first time and see hyperbaric oxygen therapy listed alongside NUCCA chiropractic and spinal decompression, it often raises an immediate question: what does a pressurized oxygen chamber have to do with back pain? It is a fair thing to wonder. HBOT has a history in wound care and diving medicine that predates most people’s awareness of it, and the idea that it might fit inside a chiropractic and spinal care practice is not immediately obvious. But once you understand what the therapy actually does at a physiological level, the connection becomes clear.
This post covers the fundamentals of hyperbaric oxygen therapy: the mechanism behind it, the conditions it has been studied for, what a session involves, and how it fits into the integrated treatment approach used at this clinic. If you have been curious but uncertain, this should answer most of your questions.
What Hyperbaric Oxygen Therapy Actually Does
The word hyperbaric simply means greater than normal atmospheric pressure. During a hyperbaric oxygen session, a patient breathes pure or highly concentrated oxygen inside a pressurized chamber, typically at 1.5 to 3 times normal atmospheric pressure. Under those conditions, the lungs can absorb significantly more oxygen than they can at standard pressure, and that oxygen dissolves directly into the blood plasma, not just into the hemoglobin in red blood cells.
That distinction matters. Under normal breathing conditions, oxygen is almost entirely carried by hemoglobin. When hemoglobin is saturated, as it typically is in healthy individuals, breathing more oxygen does not substantially increase delivery to tissues. Pressurized oxygen bypasses that ceiling by saturating the plasma itself, which can reach tissues that red blood cells cannot, including areas with reduced circulation, damaged capillary beds, or chronic inflammation.
The downstream effects of that increased oxygen availability are what make HBOT therapeutically relevant. Elevated tissue oxygen levels stimulate angiogenesis, the growth of new blood vessels in poorly perfused areas. They promote the release of stem cells and growth factors from bone marrow. They reduce inflammation by modulating cytokine activity. They accelerate collagen synthesis. And they create an environment that is hostile to anaerobic bacteria while supporting the function of immune cells that require high oxygen tension to kill pathogens effectively.
These are not speculative effects. The mechanisms above are well-documented in the biomedical literature and underpin the FDA-cleared indications for hyperbaric oxygen therapy, which currently include diabetic foot wounds, radiation tissue damage, carbon monoxide poisoning, decompression sickness, gas gangrene, and several other conditions. Research on additional applications, including traumatic brain injury, post-concussion syndrome, and inflammatory conditions, is active and ongoing.
Why Hyperbaric Therapy Fits Alongside Spinal and Structural Care
Spinal disc tissue is among the most poorly vascularized structures in the body. As discussed in the context of spinal decompression therapy, discs rely on mechanical movement to draw in nutrients because they lack a direct blood supply. This is part of why disc injuries are slow to heal and why chronic disc conditions are so persistent. Any intervention that improves tissue oxygenation in and around the spinal structures has a rational basis for supporting disc recovery.
Patients undergoing spinal decompression for herniated or degenerative discs are working to restore disc height and reduce nerve compression. Layering hyperbaric oxygen therapy on top of that mechanical treatment creates a biological environment that is more conducive to the tissue repair that decompression initiates. More oxygen in the plasma means more oxygen available to disc cells and the surrounding cartilaginous and ligamentous structures as they attempt to remodel.
The same logic applies in the context of nerve tissue. Nerves that have been chronically compressed by a herniated disc or a misaligned vertebra are oxygen-depleted and inflamed. Restoring the structural compression through NUCCA care or decompression reduces the mechanical source of that nerve irritation. HBOT accelerates the recovery of the nerve itself by flooding the surrounding tissue with the oxygen the nerve needs to heal and resume normal conduction.
This is the clinical rationale behind combining these therapies rather than offering them in isolation. Each addresses a different dimension of the same underlying problem: structural correction changes the mechanical environment, decompression restores disc loading, and hyperbaric oxygen supports the biological healing process that both of those interventions make possible.
Conditions Where Hyperbaric Oxygen Therapy Is Used
At Draper Spinal Care, HBOT is used as a component of care for patients with chronic musculoskeletal and neurological complaints, often in combination with NUCCA and decompression therapies. The specific presentations where it tends to be most useful include chronic back and neck pain with an inflammatory component, post-surgical recovery where tissue healing has been slow, nerve damage or radiculopathy accompanying disc conditions, chronic fatigue and systemic inflammation, and post-concussion or traumatic brain injury symptoms.
Post-concussion syndrome is worth addressing specifically, because it is an area of growing clinical interest in HBOT research. Concussions produce diffuse axonal injury, meaning the long projections of neurons are stretched or torn in ways that do not always show up on standard imaging but that disrupt normal brain function for weeks, months, or sometimes years. The resulting symptoms, which include cognitive fog, headache, sleep disturbance, and mood changes, reflect ongoing neuroinflammation and disrupted oxygen metabolism in affected brain tissue.
Several randomized controlled trials, including research published in PLOS ONE and the Journal of Neurotrauma, have found meaningful improvements in post-concussion symptoms following hyperbaric oxygen protocols. This is an off-label application in terms of FDA clearance, but it is supported by a growing evidence base and is increasingly used in clinical settings that treat athletes, military veterans, and others with concussion histories.
What to Expect During a Hyperbaric Oxygen Session
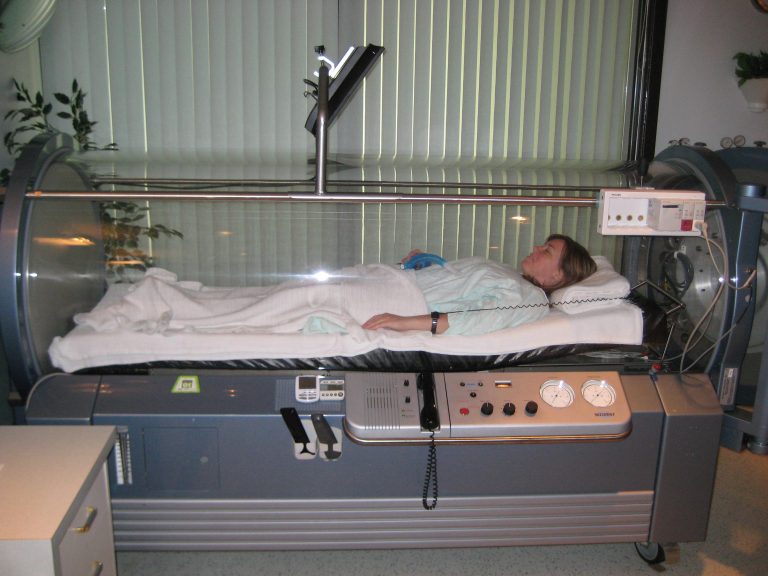
Patients enter a hyperbaric chamber and breathe oxygen at elevated pressure for a set period, typically between 60 and 90 minutes per session. The chambers used in clinical outpatient settings range from single-person, soft-sided units to rigid monoplace or multiplace chambers. The pressure inside is increased gradually at the start of the session and decreased gradually at the end, similar in feel to the pressure change when an airplane descends.
The most common sensation during pressurization is a mild fullness in the ears, which is relieved by swallowing or yawning the same way you would on a flight. Once at pressure, most patients find the session uneventful. Some read, listen to audio, or simply rest. The chamber is climate controlled and monitored throughout the session.
Treatment protocols vary by condition. A typical course for musculoskeletal or neurological applications involves multiple sessions over several weeks, often scheduled in coordination with other active therapies. The number of sessions and the pressure settings are determined during the initial consultation based on the patient’s condition, goals, and overall health status.
Safety Considerations and Who Is Not a Candidate
Hyperbaric oxygen therapy has a well-established safety profile when used within appropriate protocols and pressure ranges. Serious adverse events are uncommon. The most frequently reported side effects are mild ear or sinus discomfort during pressure changes, which resolves when pressure equalizes, and occasional lightheadedness after a session.
There are contraindications to be aware of. Patients with untreated pneumothorax should not undergo hyperbaric therapy. Certain medications, including some chemotherapy agents and bleomycin specifically, interact poorly with high-oxygen environments. Uncontrolled high fever, a history of certain ear surgeries, and severe claustrophobia are also factors that need to be evaluated prior to starting. A thorough intake and health history review is conducted before any patient begins a course of HBOT.
Patients who are pregnant, or who have a history of seizures, should discuss HBOT specifically with their primary care physician before proceeding. These are not automatic disqualifiers in every case, but they require an additional layer of medical clearance.
Learn Whether HBOT Is Right for You at Draper Spinal Care
Hyperbaric oxygen therapy is not a fringe treatment. It has decades of clinical history, a defined set of FDA-cleared applications, and an expanding evidence base across neurological, inflammatory, and musculoskeletal conditions. What makes it less familiar to most patients is simply that it has historically been confined to hospital settings. Bringing it into an outpatient spinal care clinic makes it accessible at the point of care, where it can be meaningfully integrated with the structural and mechanical therapies that address the same underlying problems from a different angle.
Not every patient at Draper Spinal Care will need or benefit from hyperbaric oxygen therapy. But for patients dealing with chronic inflammation, slow post-injury recovery, nerve-related symptoms, or post-concussion issues, it is a meaningful addition to a care plan, not a novelty.
If you are curious about whether HBOT belongs in your treatment picture, the best starting point is a conversation. Dr. Stockwell evaluates each patient’s full clinical situation before recommending any combination of therapies, and that conversation will give you a realistic sense of what to expect and whether it makes sense for you.